Childhood asthma
Children aged ≤ 5 years old
Approach to asthma in this age group are often challenging due to the various other causes that can manifest with similar symptoms as asthma e.g. viral induced wheeze. There is also lack of diagnostic test as objective testing of lung function (e.g. bronchodilator test/air flow variability) are often not feasible.
Diagnosis
Asthma diagnosis in this age group is often based on:
- Symptom patterns – recurrent ep. of wheeze, cough, SOB (often manifested by activity limitation), and nocturnal symptoms/awakening.
- Presence of risk factors – family or personal history of atopy
- Therapeutic response to controller treatment
- Exclusion of other possible diagnosis.
The table below provides guidance on the likelihood of asthma diagnosis.
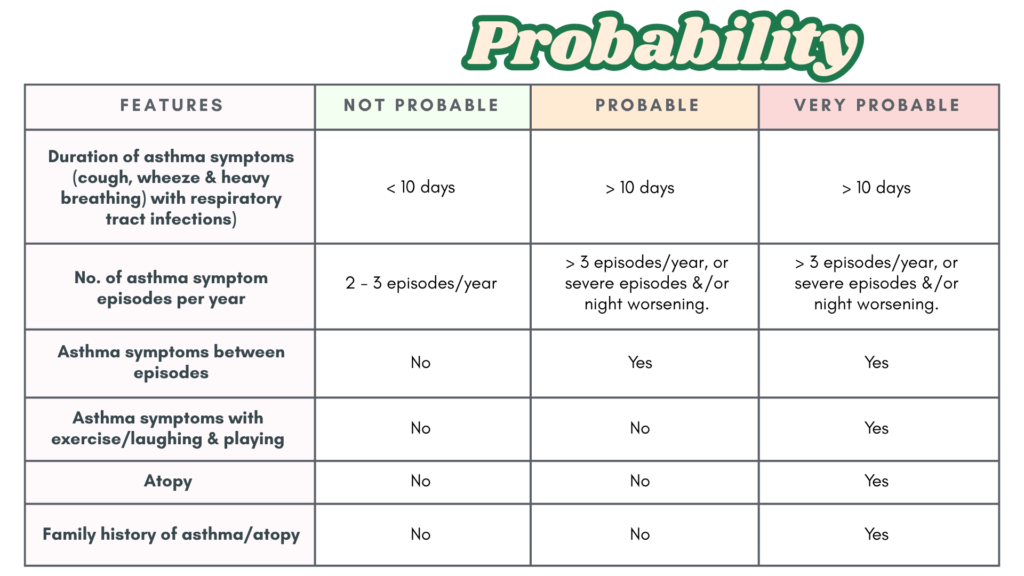
A positive family history of allergic disease or evidence of atopy in children with recurrent wheeze increases the likelihood of developing atopic asthma. Risk can be assessed using the modified Asthma Predictive Index (mAPI), which requires ≥4 wheezing episodes per year plus ≥1 major or ≥2 minor criteria.
modified Asthma Predictive Index (mAPI)
Major criteria
- Parental history of asthma (diagnosed by a physician)
- Atopic eczema (diagnosed by a physician)
- Aeroallergen sensitization
Minor criteria
- Eosinophilia ≥ 4%
- Wheezing unrelated to colds (reported by parents)
- Allergic sensitization to food, i.e. milk, egg, peanuts
Assessment
The child should be assessed as that in adults on i) asthma symptom control & ii) future risk for poor asthma outcomes.
Asthma symptom control
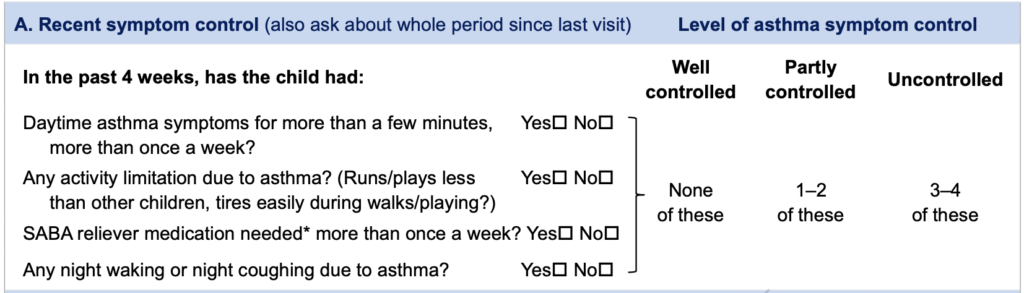
Future risk for poor asthma outcomes.

Investigations
Objective assessment (lung function tests) is difficult to perform in children ≤ 5 years as they are usually unable to perform repeatable expiratory maneuvers.
Adjuncts that can be done to support the diagnosis of asthma:
i. Chest X-ray – mainly to rule out alternate diagnosis (especially when red flags are present) like:
- Structural airway abnormalities – congenital lobar hyperinflation, vascular ring
- Chronic infections – pulmonary tuberculosis
- Chronic suppurative lung disease or bronchiectasis
- Inhaled foreign body
- Others
ii. Allergic sensitization tests – skin prick testing or allergen-specific immunoglobulin E tests.
- Allergic sensitization is the best predictor for persistent asthma.
- Nevertheless, the absence of sensitization to common aeroallergens does not rule out asthma.
Management
Management plan in this age group is based on the probability of asthma.
The goals of asthma management are similar to that of the older age groups :
- To achieve good, long-term symptom control
- Maintain normal activities
- To reduce future risks of exacerbation, impaired lung function & development
- To reduce risk of medication side effects.
Interactive diagnostic & management pathway based on the probability of asthma
Childhood Asthma (≤5 years)
Interactive diagnostic pathway for primary care: assess, classify, treat, review, and escalate when needed.
Step 1 — Clinical Assessment
Start with a detailed history and physical examination in a child with recurrent wheeze.
Treatment
Reliever therapy: inhaled SABA (pMDI salbutamol) PRN
Controller therapy:
- Daily low-dose ICS is preferred as the initial treatment. ICS should be given for at least 2 – 3 months to establish it effectiveness.
- Alternative – Montelukast (leukotriene receptor antagonist); caution regarding neuropsychiatric side effects.
There is insufficient data on the safety & effectiveness of ICS/LABA combination in < 4 years old
Inhaler devices of choice: pMDI + spacer with facemask.
ICS dosage in ≤ 5 years old
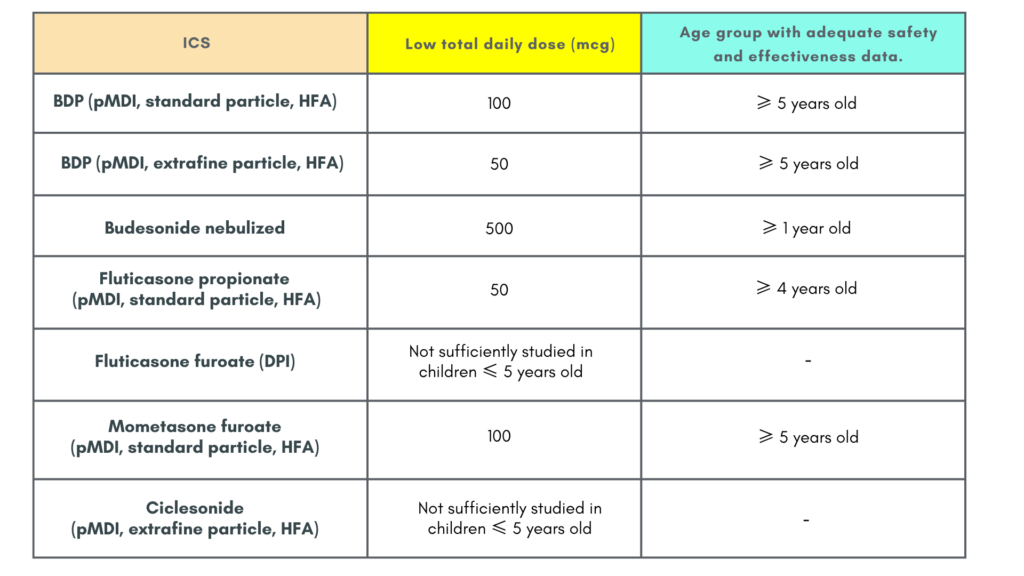
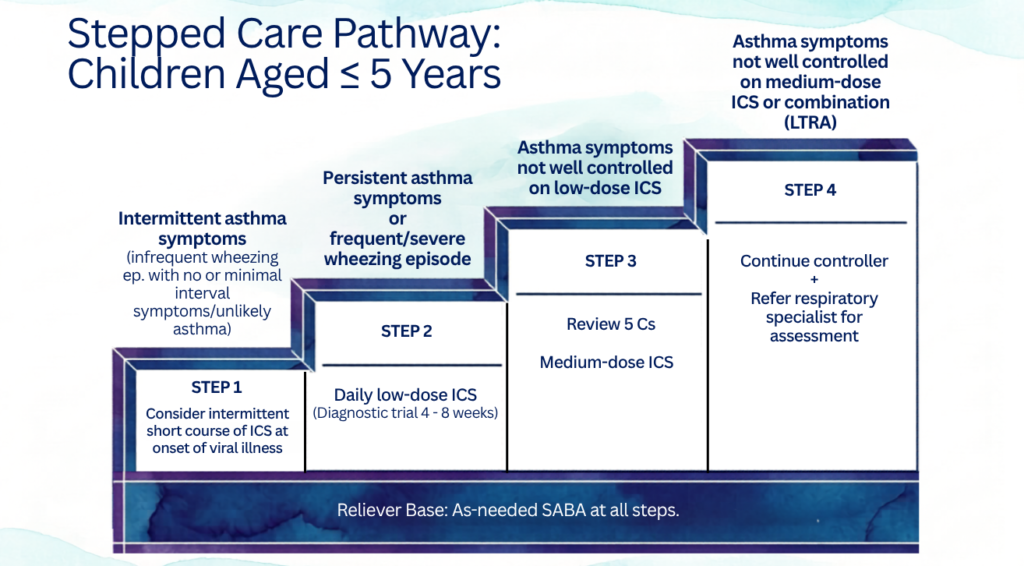
Follow up
Monitoring of symptoms in this age group are mainly based on:
- Clinical symptoms
- Childhood asthma control test (C-ACT)
- Asthma exacerbations
- Inflammatory markers – FeNO
Lung function tests are often not feasible as a tool to monitor their symptoms control.
References
- Malaysian Thoracic Society, Academy of Medicine of Malaysia, & Lung Foundation of Malaysia. (2014). Clinical practice guidelines: Management of childhood asthma.
- Global Initiative for Asthma. (2024). Global strategy for asthma management and prevention (2024 update)
