Acute Rhinosinusitis
Acute Rhinosinusitis
Definition
Rhinosinusitis is defined as an inflammation of the nose & the paranasal sinus (PNS).
Predisposing/risk factors
- Smoking (active & passive)
- Family history of chronic rhinosinusitis, asthma
- GERD
- Infection
- Allergies

Classification
Duration⌚
a) Acute rhinosinusitis(ARS):
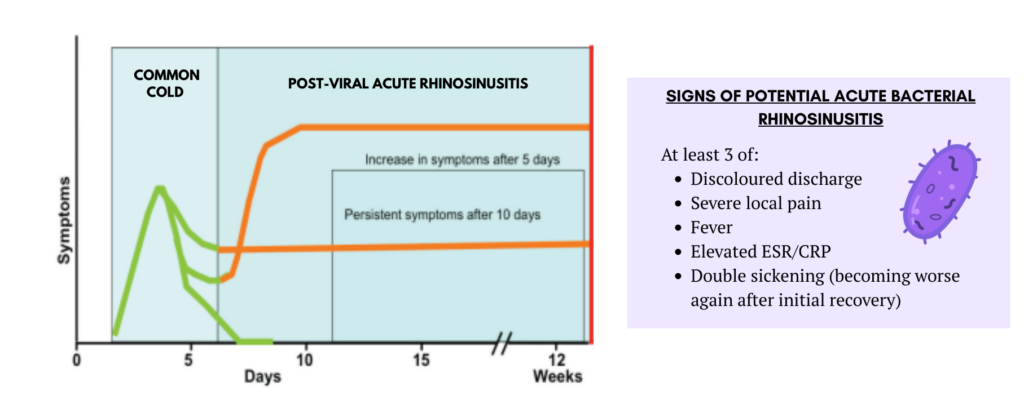
- ARS encompasses the common cold (acute viral rhinosinusitis), post-viral ARS and acute bacterial rhinosinusitis.
- Common cold : symptoms < 5 days
- Post viral ARS : increased in symptoms after 5 days, or persistence of symptoms after 10 days.
- Acute bacterial rhinosinusitis is likely when there are ≥ 3 signs and symptoms of:
– Discolored discharge (unilateral predominance) & purulent secretion in the nasal cavity
– Severe local pain (unilateral predominance)
– Fevere (> 38 °C)
– Elevated ESR/CRP
– Deterioration of SSx after recovering (‘Double Sickening’): patient often report having a cold that was getting better but then they started feeling worse again.
b) Chronic rhinosinusitis(CRS): When symptoms last > 12 weeks.
Severity
Severity of RS can be divided into the following based on total severity visual analogue scale (VAS) score
- Mild : 0 – 3
- Moderate : > 3 – 7
- Severe : > 7 – 10

Clinical presentation

Assessment
Anterior rhinoscopy should be performed as part of clinical assessment of suspected acute rhinosinusitis in primary care setting (albeit a rather limited role).
- May reveal: mucosal edema, nasal inflammation, purulent nasal discharge, polyps & anatomical abnormalities.
Nasal endoscopy should be performed to diagnosed rhinosinusitis at otorhinolaringology center (not required in diagnosing ARS in primary care)
Imaging ☢️
Plain radiograph has no role.
CT scan is the gold standard for evaluation of paranasal sinus (PNS) and is indicated when:
- Failed medical therapy
- Planned for surgery
- Atypical or severe disease or complications are suspected: unilateral symptoms, blood-stained discharge, displacement of the eye & severe pain
MRI may be useful in cases of diagnostic uncertainty or when intracranial complications are suspected.
Laboratory tests
Culture and sensitivity (C&S) may be considered in patient who do not respond to Abx treatment after 72 hours in ARS .
Nasal swab should not be performed, rather endoscopically-directed middle meatal culture should be used to obtain specimen for C&S.
Majority of ARS are viral in origin.
Common bacterial pathogen involved in RS include:
- 2 main causative agents in acute bacterial RS:
– Strep. Pneumoniae
– H. influenzae - Moraxella catarrhalis: more common in children.
- In CRS:
– Staph. aureus
– Enterobacteriaceae spp
– Pseudomonas spp - Anaerobic organisms are predominant in acute sinusitis with dental origin.
Differential diagnosis
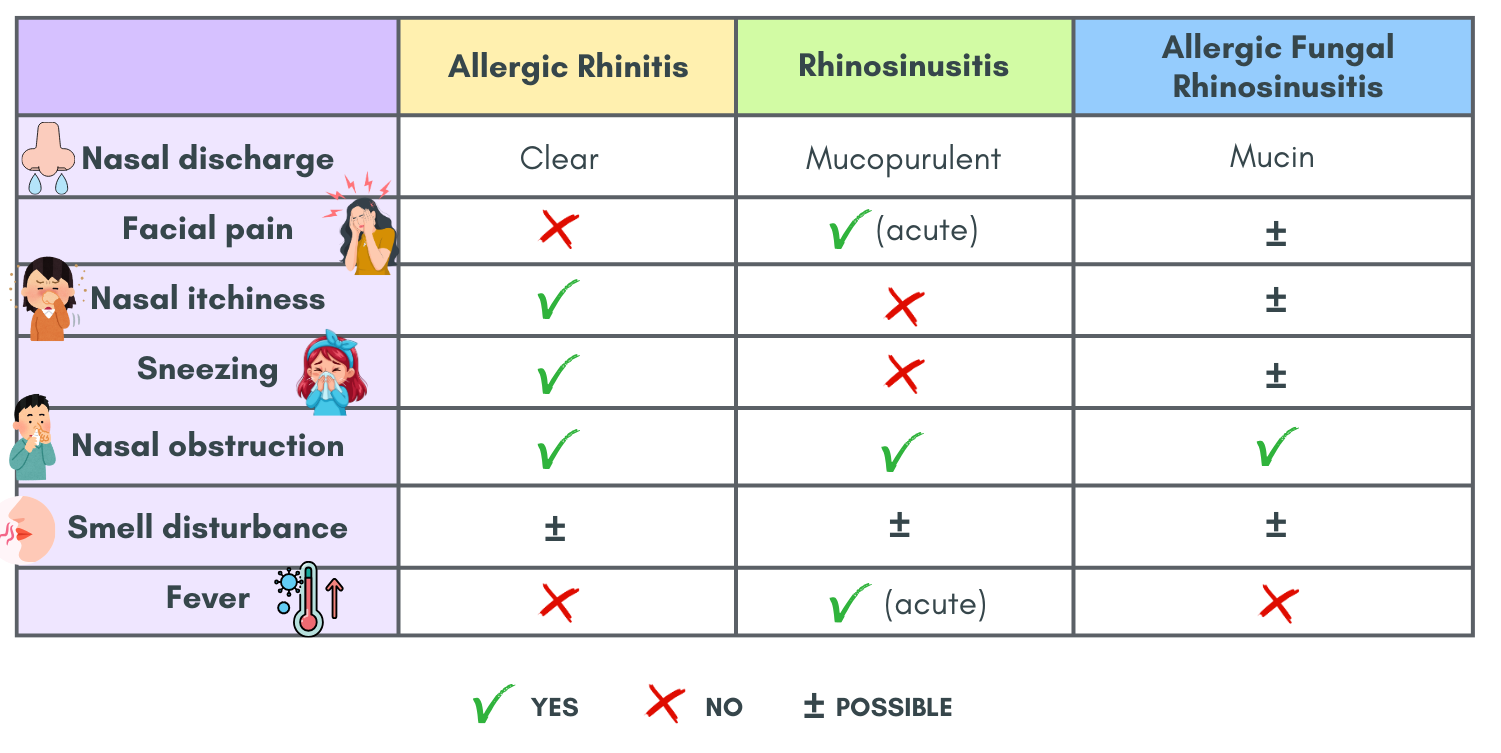
Pharmacological management
a) Antibiotics – only in acute bacterial RS
The preferred Abx:
- Amoxicillin 500 mg TDS x 5 – 7 days OR
- Augmentin 625 mg TDS x 5 – 7 days.
Abx should not be used routinely in chronic rhinosinusitis.


b) Corticosteroids
Intranasal corticosteroids (e.g. Budesonide, Fluticasone propionate, Mometasone furoate):
- Should be considered for 14 – 21 days in ARS
- Should be given for 16 – 52 weeks in CRS
Short term oral corticosteroids should ONLY be given in CRS in ORL center.
In local practice, oral corticosteroids are not given in ARS due to possibility of exacerbation of bacterial infection.
c) Nasal saline irrigation
Should be used as an adjunct therapy.
Facilitates mechanical removal of mucus, infective agents & inflammatory mediators.
Also decreases crusting in the nasal cavity & increases mucociliary clearance.
d) Antihistamines
-Should be prescribed if there are associated symptoms suggestive of allergic rhinitis (e.g. sneezing, nasal itchiness, nasal obstruction & rhinorrhoea).
e) Other medications
Analgesics: PCM or NSAIDs
Decongestants:
- Topical decongestants should not be prescribed for > 2 weeks due to rebound phenomenon.
- Oral decongestants should be cautiously prescribed in those with medical conditions e.g. DM, CV disease, glaucoma & BPH.
Treatment recommendations
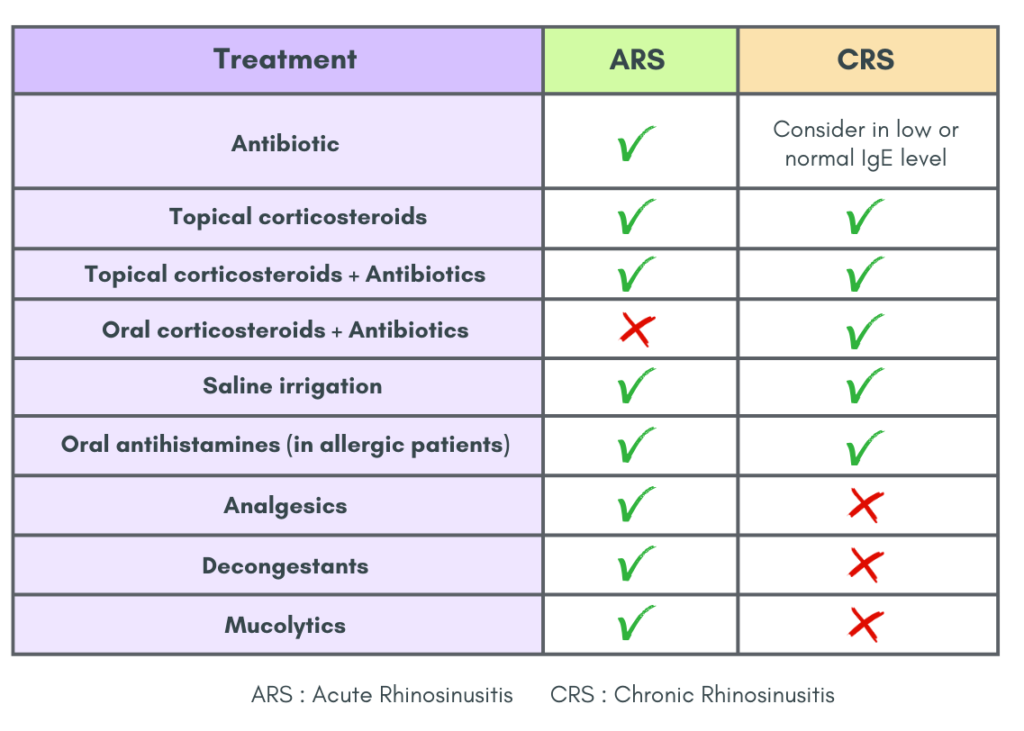
Surgical management
Indications for surgery in ARS:
- Presence of orbital or intracranial abscess on CT scan OR
- No clinical improvement after 24 – 48 hours of IV antibiotics.
Functional endoscopic sinus surgery (FESS) should be offered in patient with CRS who fail optimal medical treatment.
Algorithm
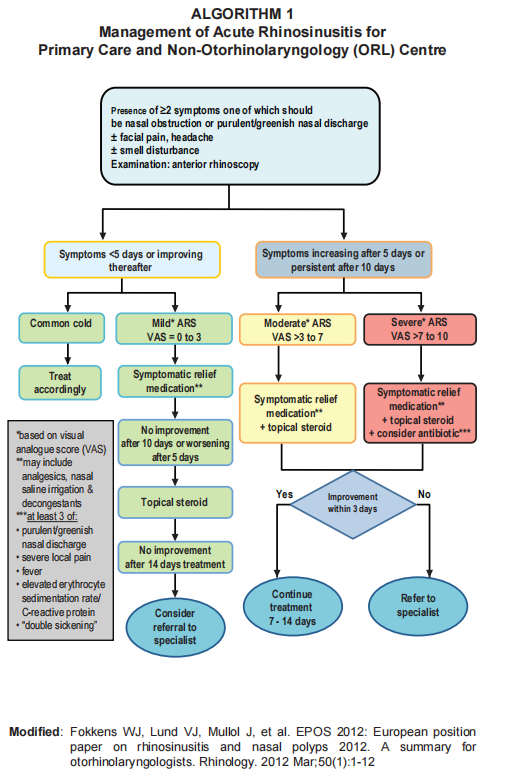
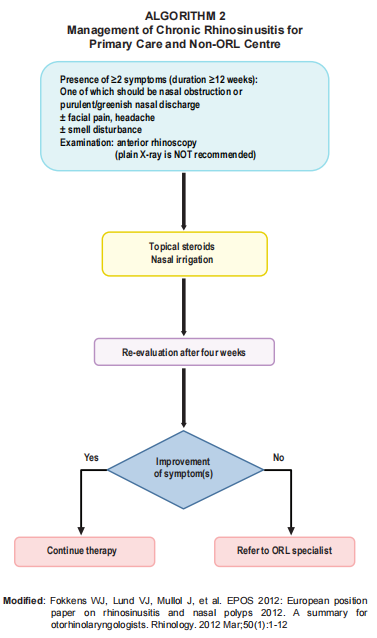
Alternative Algorithm (NAG Malaysia)
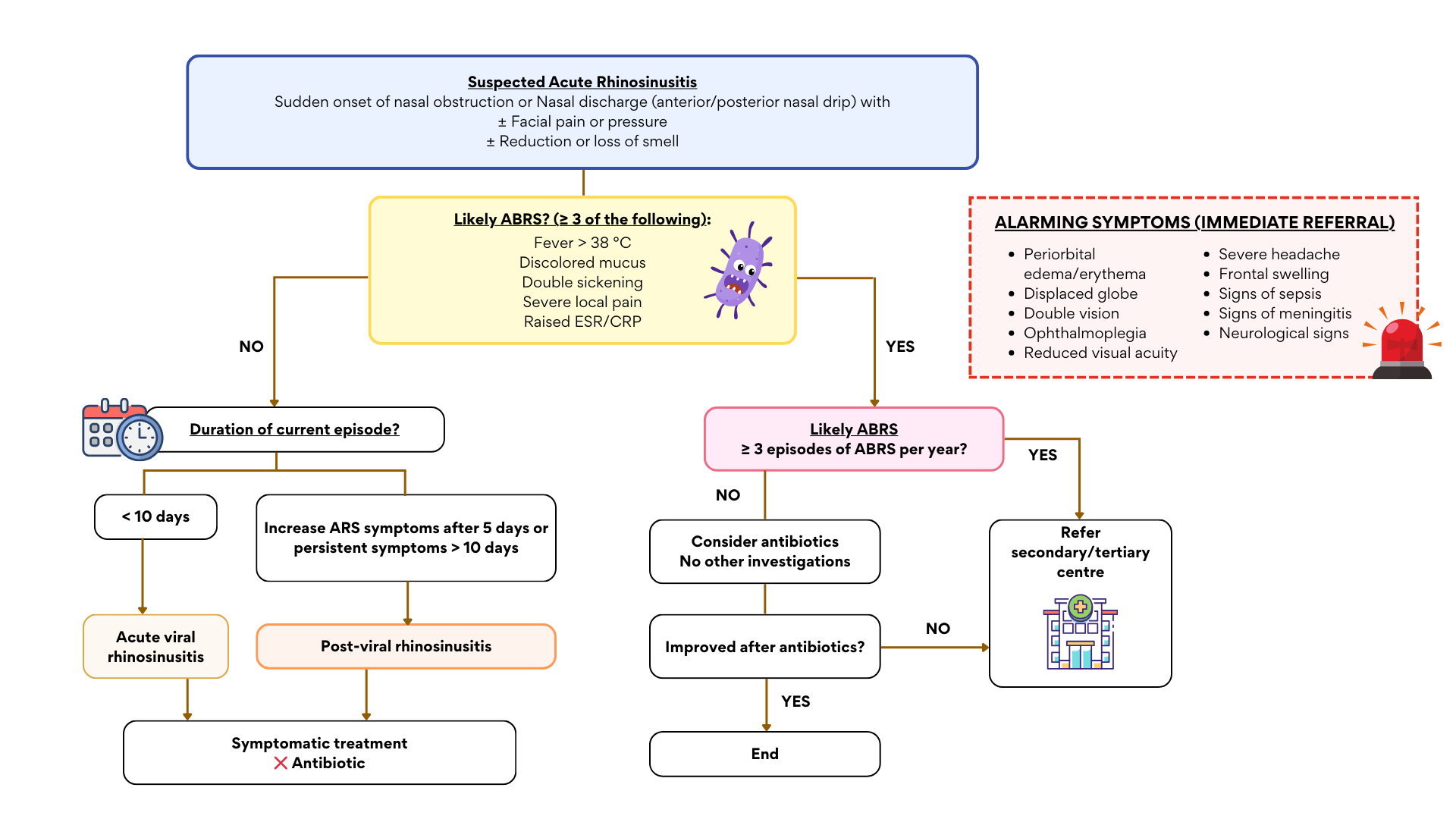
Indications of Referral
(Early referral: within 2 weeks; Urgent referral: within 24 hours)


References
- Ministry of Health Malaysia. (2017). Management of rhinosinusitis in adolescents and adults (MOH/P/PAK/340.17(GU)). Malaysia Health Technology Assessment Section (MaHTAS).
- Ministry of Health Malaysia. (2024). C4: Acute rhinosinusitis. National Antimicrobial Guideline (NAG) 2024 (4th ed.).
